Many organizations start a digital health transformation with high optimism.
They carefully select systems, prepare infrastructure, and train staff.
Then the go-live moment arrives, and the project feels finished.
However, months later, the impact is often smaller than expected.
In reality, the issue is not the technology.
In many cases, the system works well.
Instead, the real question is whether the organization changed too.
Digital Health Transformation Is Adaptation, Not Installation
An Electronic Health Record implementation study in Italy shows something important.
Low impact is rarely caused by user resistance.
Instead, it comes from adaptation behavior.
Four patterns always appear during digital health transformation.
1. Flexing The System Is Used but Adjusted
Doctors still use digital prescriptions.
However, they rewrite dosage manually.
So the system runs.
But not as designed.
This means the workflow and the system do not fully match.
2. Bypassing The System Is Skipped
If a drug is missing in the database, doctors write by hand.
As a result:
- data fragments
- audit trail disappears
- information quality drops
The transformation exists technically, but not operationally.
3. Avoiding The System Exists but Lacks Trust
Administrative staff still ask for printed copies.
The system works.
Yet trust does not exist.
Technology adoption without legitimacy fails.
4. Reorganising The Organization Changes
Some units adjust roles and coordination.
Here the real transformation happens.
The structure changes, not only the process.
Why Adaptation Is the Core of Digital Health Transformation
These patterns appear repeatedly.
Therefore adaptation is not failure.
It is part of digital health transformation.
Transformation happens when three elements align:
- technology
- clinical practice
- organization
And alignment must be led intentionally.
4 Sustainable Pillars of Digital Health Transformation
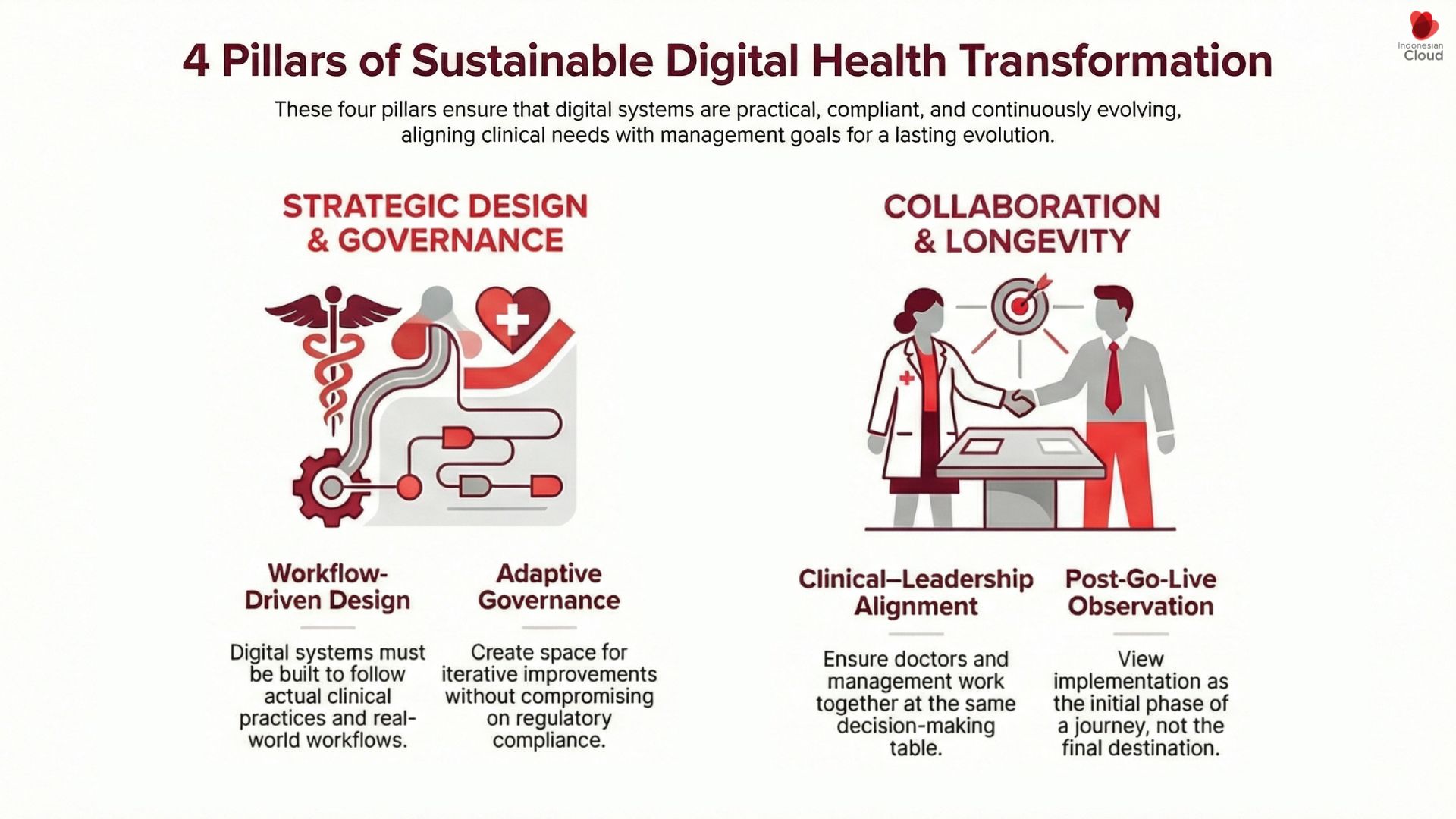
1. Workflow-Driven Design
Systems must follow real work.
If users constantly adjust the system, the design misunderstood reality.
Observation comes before configuration.
2. Adaptive Governance
Governance is learning, not only control.
User behavior gives operational insight.
Therefore organizations must allow structured iteration.
Otherwise, informal workarounds will grow.
3. Clinical-Leadership Alignment
Doctors and management must decide together.
Because digital health affects authority and accountability.
Not just IT decisions.
4. Post-Go-Live Observation
Implementation is the starting point.
Observe:
- decision changes
- data usage
- adaptation patterns
Go-live begins the operational phase.
Conclusion
In the end, digital health transformation is not a technology project. It is an organizational change process. Systems can be installed in months. Behavior change takes leadership and time. Successful organizations are not the fastest to go live. They are the ones that understand user response and align technology with clinical work. When people, systems, and decisions align, real care improvement happens. Transformation does not stop at implementation. It requires infrastructure, security, and flexibility that follow real operational needs.
PT Indonesian Cloud supports healthcare organizations with compliant, stable, and scalable cloud environments.
